
Neonatal nurse practitioners (NNPs) care for premature and critically ill neonates in neonatal intensive care units (NICU), well newborn nurseries, and special care nurseries (SCNs) within hospitals. NNPs can also work in medical transport settings, such as ground and helicopter conveyance for neonates who need emergency transport to a medical facility, as well as neonatal outpatient clinics, which follow up with premature and/or medically vulnerable infants after they are discharged from inpatient care.
NNPs work to save the lives of some of the most vulnerable patients in the medical setting. Their clinical responsibilities typically include conducting advanced health assessments, analyzing lab data, performing critical care procedures, and, in some states, writing prescriptions. They also work closely with infants’ families to provide support and education during infants’ tenure in intensive neonatal care.
The role of the neonatal nurse practitioner is intense and demanding, requiring that practitioners handle life-threatening illnesses and conditions daily, coordinate the care of delicate patients, and also manage the questions, concerns, and stress of their patients’ families. Despite these challenges, NNPs may find the positive impact their work has on the well-being of fragile neonates, the relationships they build with patients’ families, and the intellectual and physical challenges of the role to be very gratifying and energizing.
To become neonatal nurse practitioners, registered nurses must complete a graduate program with a specialization in advanced neonatal nursing from an institution that has been accredited by either the Commission on Collegiate Nursing Education (CCNE) or the Accreditation Commission for Education in Nursing (ACEN). They must also complete a minimum of 600 hours of clinical practicum in intensive neonatal care or related medical settings. After graduating from their accredited nursing program, RNs must complete a certification examination through the National Certification Corporation, and also meet state-specific licensure and/or certification requirements. After receiving all required national and state credentials to practice, NNPs should take care to maintain their license and certifications through continuing education and fulfillment of other requirements.
Where Neonatal Nurse Practitioners Work
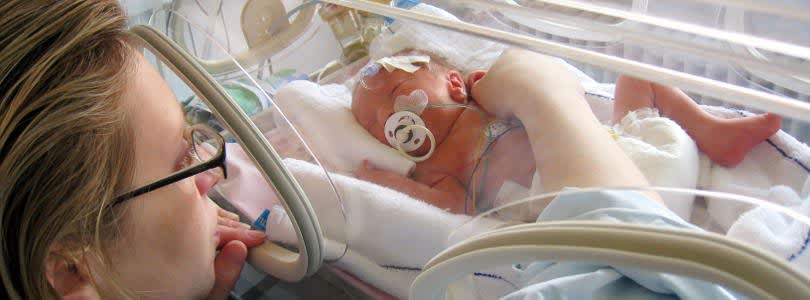 Advanced neonatal nursing is a very specialized area of critical care, involving many different medical resources and highly trained staff. As a result, neonatal nurse practitioners work almost exclusively in hospital and medical settings that specifically serve neonates and their families. Such medical environments include hospital nurseries and neonatal intensive care units, neonatal medical transport services, and outpatient infant care clinics. Below is a detailed description of several of the main medical settings that employ neonatal nurse practitioners.
Advanced neonatal nursing is a very specialized area of critical care, involving many different medical resources and highly trained staff. As a result, neonatal nurse practitioners work almost exclusively in hospital and medical settings that specifically serve neonates and their families. Such medical environments include hospital nurseries and neonatal intensive care units, neonatal medical transport services, and outpatient infant care clinics. Below is a detailed description of several of the main medical settings that employ neonatal nurse practitioners.
Hospital Neonatal Intensive Care Units (NICUs) and Nurseries
According to the American Academy of Pediatrics, neonatal care in the United States is divided into four distinct levels of care. Hospitals must earn state licensure in order to designate themselves as a particular level of NICU or SCN. Different states may have specific staff, equipment, and medical care requirements for each level of neonatal care; however, the types of care that each level of neonatal care provides tends to be fairly consistent nationwide. Neonatal nurse practitioners may work at one or more levels in one hospital, or rotate between several hospitals across multiple levels of advanced neonatal care. Below is a more detailed description of the different levels of neonatal care offered in hospital settings.
Level I (Well Newborn Nursery)
The Level I nursery is often called the well newborn nursery, and is typically reserved for both healthy babies and infants who are ill but in stable condition. The Level I nursery also houses infants who are younger than 35 weeks gestation who need to wait to be transferred to another facility that can provide a higher level of care. Level I NICU nurseries have the equipment and the staff to provide neonatal resuscitation if necessary at every delivery, and can also provide thorough post-natal health evaluations and care to newborns.
Level II (Special Care Nursery)
The Level II neonatal nursery, also called the special care nursery, offers all the services that Level I nurseries provide, as well as additional services to support neonates who were born at greater than 32 weeks gestation and who are suffering from moderate health conditions or are recovering from more serious ailments. Most Level II nurseries have the equipment and staff necessary to provide moderate respiratory support or stabilization, including continuous positive airway pressure (CPAP) and/or mechanical ventilation. Level II nurseries also have the equipment and staff to stabilize infants born before 32 weeks gestation and weighing less than 1500 grams until they can be transferred to a neonatal intensive care unit.
Level III (NICU)
In addition to providing all the care that Level I and II nurseries provide, Level III NICUs must have ready access to a full range of pediatric medical and surgical subspecialists, pediatric anesthesiologists, and pediatric ophthalmologists. Level III NICUs must have the resources to provide sustained life support and comprehensive care to infants suffering from critical illness, and infants who are younger than 32 weeks and weigh less than 1500 grams. Level III NICUs also provide a wider range of respiratory support and advanced imaging services.
Terri Jo Peterson, MSN, NNP-BC, is a Neonatal Nurse Practitioner who works in the Level III NICU at Hennepin County Medical Center, where she coordinates the care of critically ill infants and micro-preemies (defined as an infant weighing less than 700-800 grams and are younger than 26 weeks gestation). “At the Level 3 NICUs, I work with micro-preemies to term infants who are in the NICU for various reasons. The micro-preemies are of course, having respiratory distress and need support both with respiratory issues and numerous other issues during their prolonged stays in the NICUs,” she explained, “Term infants also can have respiratory problems, infection, neurological issues, electrolyte issues, and hypoglycemia. Infants can also experience Neonatal Abstinence Syndrome, a condition that may occur when pregnant women take drugs such as heroin, codeine, methadone, oxycodone, and buprenorphine.”
Level IV (NICU)
Level IV NICUs offer the highest level of care to neonates. In addition to providing all the care that Level III NICUs provide, Level IV nurseries have surgical subspecialists, medical subspecialists, and anesthesiologists on site who are trained to address complex congenital and acquired neonatal conditions. Level IV NICUs can also facilitate medical transport of neonates and can engage in outreach education within the community.
Neonatal Medical Transport Teams
Ground and helicopter transport of critically ill and high-risk neonates requires a highly trained and specialized team, including neonatologists, specialized transport nurses, and neonatal nurse practitioners. Neonatal nurse practitioners who are on medical transport teams need to work skillfully in fast-paced, high-acuity settings. Neonates struggling with a severe health condition that cannot be treated at the location where they have been born must be quickly and safely transferred to a tertiary care center that can meet their needs. Timing is crucial, as shorter transport time typically leads to better health outcomes.
Jenny Quinn, MSN, NNP-BC is a Neonatal Nurse Practitioner and Clinical Practice Manager at Northbay Healthcare who worked for several years as an NNP at the University of California, San Francisco’s (UCSF) Benioff Children’s Hospital. In an interview with OnlineFNPPrograms.com, she explained her role on the neonatal transport team at UCSF. “I was also a member of the neonatal transport team and provided medical management for critically ill infants on ground, fixed-wing and helicopter transports within Northern California,” she said, “The neonatal transport team consisted of me and a NICU nurse; the goal of transport is to stabilize an infant prior to leaving the referring hospital but many times an infant would decompensate en route to UCSF and we would support the infant as best as possible in a limited space such as in the back of an ambulance, helicopter or small airplane. Not only is there limited space but limited personnel and equipment; constant assessment of an infant during transport is thus critically important in properly managing during transport.”
Educational Settings
In addition to working directly with patients in nursery, NICU, and medical transport settings, neonatal nurse practitioners can work in educational settings both in hospitals and university and nursing school settings. Dr. Mary Puchalski, MSN, DNP, NNP-BC is the Director of the Neonatal Nurse Practitioner (NNP) program at the University of Illinois at Chicago College of Nursing, where she also teaches as an Assistant Professor. “As a faculty member and director of the NNP program at the University of Illinois at Chicago, I am responsible for the development, provision, and support of the curriculum preparing registered nurses to obtain a Doctor of Nursing Practice degree and a specialty concentration in advanced practice neonatal nursing as a nurse practitioner,” she said, “I also advise all students in the NNP specialty and support the development, implementation, and evaluation of their DNP projects in the clinical arena.”
Prior to becoming a professor, Dr. Puchalski was the Perinatal Outreach Education Coordinator at Loyola University Chicago’s Perinatal Center, which gave her the opportunity to develop educational programs and conduct outreach to hospitals within Loyola’s network. “As an Outreach Education Coordinator I provided educational programming and support, and quality improvement activities for the Loyola Perinatal Center network hospitals for perinatal nursing providers,” she explained. This role involved evaluating the training needs of staff at various hospitals, creating curricula that met these needs, and also staying up-to-date on national and state requirements for competency in the field. “I performed needs assessments with the nursing staff of the network hospitals to identify critical learning needs, designed educational programs to meet those needs, and provided updates on national and local practice policies and competencies. Some of the programs I supported include AWHONN’s fetal monitoring program, the AAP Neonatal Resuscitation Program (NRP), and the S.T.A.B.L.E. Program,” she said, “I was also responsible for maintaining relationships with the stakeholders, both within the perinatal center and network hospitals.”
What Neonatal Nurse Practitioners Do
 Neonatal nurse practitioners provide a wide range of intensive and timely medical services to neonates at various levels and stages of illness. They specialize in preterm and newborn infants, but can also treat children up to two years of age. Their daily clinical work can include attending high risk deliveries, performing advanced procedures before, during, and after an infant’s birth, and providing individualized management of ill neonates in the NICU. Below is a more detailed description of some of the core responsibilities that neonatal nurse practitioners have in clinical and educational settings.
Neonatal nurse practitioners provide a wide range of intensive and timely medical services to neonates at various levels and stages of illness. They specialize in preterm and newborn infants, but can also treat children up to two years of age. Their daily clinical work can include attending high risk deliveries, performing advanced procedures before, during, and after an infant’s birth, and providing individualized management of ill neonates in the NICU. Below is a more detailed description of some of the core responsibilities that neonatal nurse practitioners have in clinical and educational settings.
Health Assessments
Neonatal nurse practitioners complete physical assessments of neonates upon their admission into a nursery or NICU, and also conduct regular health evaluations throughout their patients’ tenure in the hospital to ensure proper stabilization and recovery. Marla Conley, MSN, NNP-BC is a Neonatal Nurse Practitioner at Kosair Children’s Hospital Neonatal Specialists, where she cares for fragile neonates in the NICU. In an interview with OnlineFNPPrograms.com, she explained how detailed health assessments are an important part of developing an effective ongoing plan of care for her patients. “Each day, my responsibility includes assessing each baby, reviewing the history, and interpreting laboratory and radiographic results,” she said, “I then use this data to make a plan for each baby.”
Neonatal physical assessments can involve evaluating all of a patient’s major body systems, including respiratory, digestive, cardiovascular, muscular, and nervous. The data collected during these evaluations is crucial to designing an effective plan of care that combines nutritional planning, respiratory and cardiovascular support services, and monitoring of patient growth and stabilization. “Nutrition will play a key role in a premature baby’s short and long term plan,” Ms. Conley said, “Each day, I will do a nutritional assessment, which includes interpreting lab values, conducting growth assessments, and calculating calories needed for this baby to grow considering environmental challenges and physiologic challenges that come with prematurity.”
Targeted Treatments and Procedures
Neonatal nurse practitioners attend high-risk deliveries alongside physicians and nurse midwives, and help to address complications during and after birth. They perform delicate procedures such as intubations and extubations, percutaneous arterial line and central line placements, umbilical catheter placement, chest tube insertions, and lumbar punctures. After a baby is admitted into a neonatal intensive care unit, he or she is monitored on a daily basis and given proper nutrition and medical support to stabilize his or her conditions. “I will attempt each day to provide [each] baby with nutrition, via total parenteral nutrition (TPN) and lipids and/or milk feedings that mimic in utero nourishment to the best of my ability,” Ms. Conley said of her daily work with patients.
Working in the NICU requires daily management of patients and continual monitoring of their progress. “I will address each problem every day and attempt to advance my babies toward stabilization. I manage their respiratory system by ventilator adjustments based on their assessment, intubations or extubations, X-ray interpretations and changes in oxygen delivery as needed,” Ms. Conley said, “Many premature babies need cardiac or hemodynamic interventions, and I assess for changes each day and make decisions based on their needs.”
Care Coordination
Neonatal nurse practitioners operate as part of a larger team of health care practitioners and medical staff. “It is incredibly humbling when you encounter a parent outside of the hospital and they thank you for all you did for their child because you know it took ‘a village’ to accomplish it,” Dr. Puchalski said in her interview with OnlineFNPPrograms.com, “All patient management and care is delivered in collaboration with attending neonatologists, the bedside nurse, and other interdisciplinary team members.”
NNPs meet frequently with neonatologists, registered nurses, and other members of their medical team to review patients’ health statuses and to develop or update their patients’ plans of care. “Our team at Kosair Children’s Hospital includes neonatologists and nurse practitioners. We also have pharmacists who are specially trained in neonatology who assist us, speech pathologists that assess and treat feeding/mechanical problems, and nutritionists specially trained in neonatology as well as physical therapy and occupational therapy,” Ms. Conley said, “We also have discharge planners that work closely with us and with the families in preparation for discharge needs. We work together and meet once a week to discuss the overall plans.”
NNPs can take on leadership roles within the medical setting, managing the logistics of patient admission and discharge, supervising and training nursing staff and residents, and acting as the connection between patient, family, and the medical team. “In my roles as Lead NNP at the Level 2 NICU at two of Allina’s hospitals, […] I acted like a liaison between the nursing and NNP staff with neonatology and pediatrics,” Ms. Peterson said, “I was responsible for making sure all the NNPs had their hospital based annual training completed along with their NRP and CRP certificates up to date.” When necessary, NNPs are also in communication with social workers, hospital chaplains, and outpatient care facilities to ensure that patients and their families receive external support before, during, and after their transition from hospital-based care to either outpatient care or home.
Neonatal nurse practitioners may find opportunities to expand their administrative and care coordination responsibilities by working with physicians and administrators to improve hospital policies and procedures. After her position at UCSF, Ms. Quinn assumed a role as a Clinical Practice Manager and Neonatal Nurse Practitioner at Northbay Healthcare. “As CPM, I have authority and accountability for the orientation and educational offerings provided to not only the NICU nurses but also medical/surgical nurses that can care for stable neonates, for example neonates with hyperbilirubinemia requiring phototherapy,” she told OnlineFNPPrograms.com, “I also collaborate closely with the Neonatologists and Pediatricians in the development of clinical practice policies and procedures. This requires research on current evidence or best practices and integrating this information into policies and procedures.”
Family Support and Education
The family-centered care that is central to neonatology means that NNPs and other medical staff communicate regularly with patients’ families, and involve them as much as possible in the care of their child. “In my facility, we strive to include the parents in the care and planning of their child’s medical management. We make contact with them at least once a day to update them, to allow for questions, and to discuss the plan for their child that day,” Ms. Conley noted, “We encourage their participation in daily hands-on care as well. Many of our rooms are private and the parents are encouraged to stay with their baby or babies.”
The support of patients’ families also includes educating them and preparing them for complications before, during, and after the delivery of their child. “During my shifts, I […] speak with mothers who come in to the hospital with preterm labor about what will happen at their delivery, and discuss all potential problems that may occur in the infant from head to toe going by systems,” Ms. Peterson told OnlineFNPPrograms.com.
Educating infants’ families can help optimize patient outcomes by enabling parents to maintain a connection with their child during his or her tenure in the NICU, solidifying the partnership between families and the medical team, and ensuring that parents are well-informed about how to care for their infant after he or she leaves the hospital. “[Neonatal nurse practitioners] provide parent/family support, anticipatory guidance, and education as families are considered integral partners in the care of their infant,” Dr. Puchalski noted.
Staff Education and Program Development
As mentioned previously, neonatal nurse practitioners can also help design and run hospital-based education programs for physicians, nurses, and other medical staff. During her time at UCSF, Ms. Quinn also worked as a Neonatal Outreach Coordinator, developing and implementing advanced curricula at numerous outreach hospitals with the aim of teaching nurses, physicians, and medical staff about effective management of neonatal conditions such as neonatal sepsis, developmental issues, and meconium aspiration. She also designed and implemented NICU simulations and presentations on neonatal care topics and national treatment standards. Dr. Puchalski’s position as an Outreach Education Coordinator at Loyola University Chicago offered her similar opportunities to design and implement educational programs to meet the needs of perinatal nurses at several hospitals. Neonatal nurse practitioners with several years of clinical experience and a desire to engage in staff trainings and program development may find opportunities by speaking with nurse leadership at their hospital, and by volunteering to take on additional tasks that help them to gain experience in program development, curriculum development, and educational outreach.
The Rewards and Challenges of Advanced Practice Neonatal Nursing
 Advanced practice neonatal nursing is one of the most challenging fields of nursing, due to the fragility of the patients and their need for intensive, constant, and comprehensive medical care. Yet the rewards of the profession can be equal in measure to the demands of the daily work. Neonatal nurse practitioners work closely with families during some of the most trying experiences of their lives, and have the opportunity to bring some of the most vulnerable patients in the medical setting back into safety and well-being.
Advanced practice neonatal nursing is one of the most challenging fields of nursing, due to the fragility of the patients and their need for intensive, constant, and comprehensive medical care. Yet the rewards of the profession can be equal in measure to the demands of the daily work. Neonatal nurse practitioners work closely with families during some of the most trying experiences of their lives, and have the opportunity to bring some of the most vulnerable patients in the medical setting back into safety and well-being.
“The field of advanced neonatal nursing is so very rewarding. When you take care of a premature baby, weighing only 500 grams in the beginning, the family goes through so many ups and downs during their stay in the NICU,” Ms. Conley said, “You establish a trusting relationship with the parents and they look to you to take care of their most precious possession. You rejoice with them on the good days and cry with them on the bad. But in the end, when I see these babies going home healthy, I feel so good about the fact I played a role in the success. That is an awesome feeling.”
The relationships they form with patients’ families and the ability to give parents emotional support, a voice in the care of their child, and empowering knowledge about their baby’s condition are reasons many NNPs find the work they do to be fulfilling and energizing. “Working in the NICU, you not only care for an extremely premature infant who weighs less than a pound or the term infant with meconium aspiration syndrome, but you’re also taking care of that infant’s family,” said Ms. Quinn, “The trust that parent(s) give you, the role I play in empowering and teaching the parents to discover their baby’s cues and ultimately to wish them well upon discharge are all huge satisfiers as a NICU nurse.”
Working as a neonatal nurse practitioner may also provide many opportunities for professional and personal growth due to the challenging, multifaceted, and simultaneously collaborative and independent nature of the role. “The level of autonomy, decision-making, collaborating and project development has been very fulfilling for me professionally. Many doorways open up if you are willing to push yourself beyond your comfort level and become involved in your profession,” Ms. Quinn added.
Challenges of the profession include emotional pain when a patient’s condition worsens, and the risk of overwork due to on-call hours, night shifts, and the intense nature of the daily tasks required. “Challenges come in numerous forms, many of which are common to any workplace: differences in individual knowledge, practice/treatment preferences, and personalities,” Dr. Puchalski noted, “The long workday hours and in-house call requirements of a clinically based NNP can also be challenging, both in balancing one’s personal life and health, as well as professional life and health. Some of these challenges are exacerbated by the aging process.”
Neonatal care environments can be fast-paced, and the fragility of the patients means that their health can decline rapidly. Working in such an environment requires quick thinking and constant collaboration among health care providers. “Prioritization is a huge part of the job, especially during times of high acuity and a high number of occupied beds,” Ms. Peterson said, “You could have 2 infants who self-extubate at the same time and you need to respond to the one that is not tolerating bag mask ventilation before intubating the second child. The other thing is to know when and whom you need to call for help or to have questions answered.”
Ms. Quinn advises that new and prospective neonatal nurse practitioners maintain a healthy separation between their professional life and their work life, and to seek support systems among their colleagues and social groups. “One of the challenges is maintaining a healthy work perspective. It can be mentally exhausting working with critically ill infants, their parents and families, and unfortunately some infants will die, which presents an incredible challenge for all family members and medical professionals involved,” she said, “On a personal level, I try not to take my work home with me. That is a very common adage, but it has helped me throughout my career. […] In those occurrences when a baby unfortunately dies, and one has in every hospital I’ve worked in, there has been wonderful assistance from management, nursing and physician colleagues and spiritual services.”
Advice for Registered Nurses Who Wish to Become Neonatal Nurse Practitioners
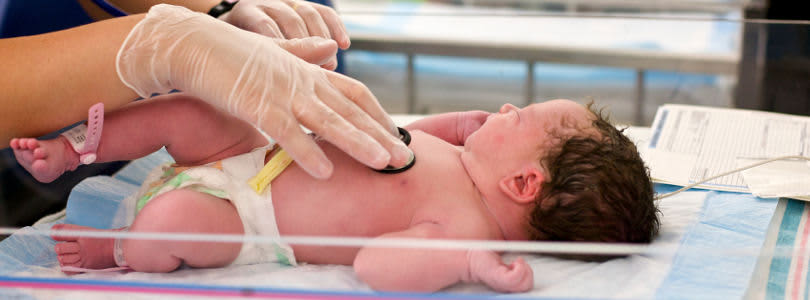 Registered nurses and nursing students who are interested in becoming neonatal nurse practitioners must enroll in a graduate nursing program specializing in advanced neonatal nursing that has been accredited by either the Commission on Collegiate Nursing Education (CCNE) or the Accreditation Commission for Education in Nursing (ACEN). They must also complete more than 600 hours of clinical practicum hours in settings that prepare them for work in the NICU. Certification to become a neonatal nurse practitioner is provided through the National Certification Corporation (NCC).
Registered nurses and nursing students who are interested in becoming neonatal nurse practitioners must enroll in a graduate nursing program specializing in advanced neonatal nursing that has been accredited by either the Commission on Collegiate Nursing Education (CCNE) or the Accreditation Commission for Education in Nursing (ACEN). They must also complete more than 600 hours of clinical practicum hours in settings that prepare them for work in the NICU. Certification to become a neonatal nurse practitioner is provided through the National Certification Corporation (NCC).
In addition to obtaining on-the-job experience in neonatal care settings during their time as an RN and completing a graduate program that fulfills the NCC’s requirements for certification, prospective NNPs should seek out relevant volunteer opportunities and connect with fellow students and practitioners through professional associations. Being proactive, observant, ready to engage in varied work, and eager to learn as much as possible can help one succeed and grow in this field.
“You’ll never stop learning and the more you can absorb from those willing to teach, the better–take advantage of those opportunities. If you are working in a NICU, volunteer for projects or participate in a unit committee. This may give you an opportunity to learn about project development and management and also collaborate with other disciplines to attain a goal or objective,” Ms. Quinn advised.
Dr. Puchalski similarly advised registered nurses and nursing students pursuing a career in advanced neonatal nursing to stay apprised of developments in the field by joining relevant professional organizations and reading journals on neonatal care. “Membership in the National Association of Neonatal Nurses (NANN) and their local chapter, attendance in the educational activities of these organizations, and reading the journal [Advances in Neonatal Care] will enhance [prospective NNPs’] professional portfolio.” She also encouraged prospective NNPs to seek out volunteer opportunities to build their leadership skills and experience, noting, “Numerous volunteer activities are available through one’s local chapter of the March of Dimes. Additionally, participation in your organization’s nursing committee demonstrates leadership potential.”
For nurses who are interested in becoming nurse practitioners and who are currently employed at a NICU, Ms. Conley recommends asking questions and trying to understand the care coordination side of neonatal care. “Understand the day to day management. Talk to your pharmacists and nutritionists if possible. Learn why this antibiotic or formula concoction was started and not another,” she said, “If you have a baby with a certain defect or condition, go read about it that day, it will make more sense to you and you will remember it better. The NNP boards is all about management: fluids and electrolytes. Understand why total fluids were or were not advanced for your baby that day. Understand who gets higher fluids and who is fluid restricted. Understand why certain tests were ordered. Pay attention and ask questions!”
As mentioned previously, neonatal nursing is a challenging field, and can be particularly draining when one has assumed a more advanced role as a care provider, which involves more management and leadership in addition to clinical responsibilities. Neonatal nurse practitioners should develop and maintain a strong support system and self-care plan that can help them reduce fatigue and stress. “For those considering a neonatal nurse practitioner career, you must realize it is very demanding and often comes with long hours, working weekends and holidays,” Ms. Conley noted, “To be honest, the times I have questioned my decision, was because of time missed with family and my children due to my schedule. As I said, I love my profession, but it comes with a demanding schedule as most jobs do in the medical profession.”
With adequate academic and professional preparation, a resilient and compassionate attitude, and a strong support network, neonatal nurse practitioners can create a highly rewarding career path that allows them complete impactful work on a daily basis amongst colleagues who are similarly motivated to help vulnerable infants achieve and maintain health and wellness. “I love my job as a neonatal nurse practitioner,” Ms. Conley said in her interview, “I have never regretted my career decision. I get to learn and use my brain every minute of every workday. I feel rewarded and challenged. The field of neonatology is special. The professionals I currently work with and have worked with in the past are the most caring and sensitive men and women I have every encountered; not to mention the most intelligent group of professionals ever! I am so very proud to be in a profession with members who devote themselves to our tiniest and most vulnerable patients!”
Sources:
- “Levels of Neonatal Care,” floyd.org, Floyd Medical Center, https://www.floyd.org/medical-services/maternity/NICU/Pages/Levels-of-Neonatal-Care.aspx
- “Levels of Neonatal Care,” pediatrics.aappublications.org, American Academy of Pediatrics, 2004, http://pediatrics.aappublications.org/content/114/5/1341
- “Washington State Perinatal and Neonatal Level of Care (LOC) Guidelines,” doh.wa.gov, Washington State Department of Health, February 2013, https://www.doh.wa.gov/Portals/1/Documents/Pubs/950154.pdf
- “NICU Tests and Procedures,” mottchildren.org, C.S. Mott Children’s Hospital, https://www.mottchildren.org/conditions-treatments/nicu-tests-and-procedures#picc

